A commonly asked question we get at the Male Fertility and Peyronie’s Clinic is whether the use of surgical drains in the scrotum during a vasectomy reversal will improve the outcome of the surgery. This article will review what drains are and whether they impact outcomes of vasectomy reversals.
What is a Surgical Drain?
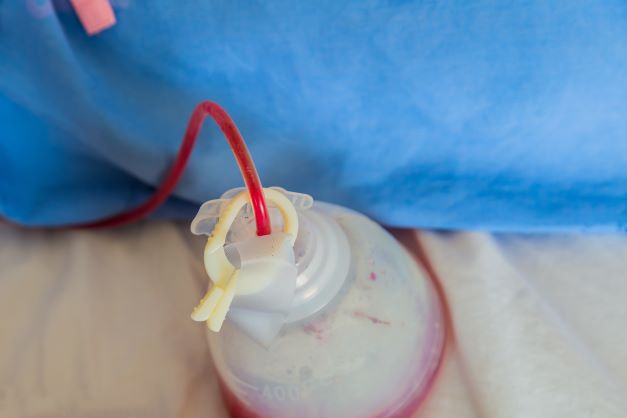
A drain is a medical device which is placed at the time of surgery and removed at a later date. One example of a commonly used surgical drain is shown in the accompanying picture. The drains are typically made of silicone or other synthetic materials, and the goal of placing a drain is to cut down on the amount of fluid which builds up at the surgical site. Drains are commonly used with certain types of surgeries, such as those performed in the abdomen. However, their use with scrotal surgeries remains controversial.
Do Vasectomy Reversal Surgeons Use Drains?
Although no studies have specifically reported the percentage of surgeons which use drains at the time of a vasectomy reversal, in general, it is not a common procedure for most reversal surgeons. Some surgeons use them in selective cases, while others may use them in all cases. However, the majority of reversal surgeons do not use drains post-operatively.
Do Drains Improve Outcomes of Vasectomy Reversals?
The short answer is that no one knows for sure. The longer answer is a bit more nuanced. In reviewing the published scientific literature, there are currently no studies which have specifically compared outcomes between vasectomy reversal cases that did or did not use a drain. Because of this lack of data available, we extended our search into other similar surgeries in the scrotum where a scrotal drain might be used.
Two surgeries which are commonly done in the scrotum and involve the testicles are hydrocelectomies and spermatocelectomies. These surgeries have a relatively high complication rate, including hematomas (large blood collections) and seromas (non-bloody fluid collection). Dr. Kiddoo and colleagues did a research study evaluating outcomes of men undergoing these surgeries with or without the use of surgical drains. The study included 161 patients and spanned from April 1, 1997 to March 31, 1999 at one institution. The average age of the patients was 53.7 years old, and the overall complication rate was 19.2% (9.3% infection/scrotal abscess, 9.3% persistent swelling, 0.6% chronic pain). In comparing whether drains made a difference in complication rates, they found that overall, drains did not make any difference (not better or worse).[i] Other studies evaluating scrotal surgeries have similarly demonstrated no benefits with the use of a scrotal drain.[ii]
There is currently a randomized clinical trial under way to determine the efficacy of closed suction drains during a hydrocelectomy. The study will determine the benefit or lack of benefit when putting a closed suction drain in during hydrocele surgery. The objective is to compare postoperative complication rates between patients with and without closed suction drains as well as compare postoperative pain between the two groups. This study was set to be completed by August 1, 2022, however, no data are currently available on outcomes.[iii]
Summary
Overall, further studies are needed to determine whether the use of scrotal drains in vasectomy reversal surgery is beneficial and worth the extra hassle and scarring for patients. Without any studies specifically comparing outcomes with and without drains, it is not possible to say if they are beneficial or not. In general, our opinion is that drains do not offer any clear benefits post reversal, and, given the extra hassle for patients, skin scarring (site of placement in the skin), potential risk that the drain gets caught or pulls on the surgical repair, and available data in other surgeries showing no reductions in post-operative complication rates, we do not routinely recommend or place them.
[i] Kiddoo, D.A., Wollin, T.A., and Mador, D.R. (2004). A population based assessment of complications following outpatient hydrocelectomy and spermatocelectomy. J Urol., 171(2 Pt 1), 746-8. DOI: 10.1097/01.ju.0000103636.61790.43 https://pubmed.ncbi.nlm.nih.gov/14713801/
[ii] Swartz M.A., Morgan T.M., and Krieger J.M. (2007). Complications of scrotal surgery for benign conditions. Urology, 69(4), 616-9. https://pubmed.ncbi.nlm.nih.gov/17445635/
[iii] Sasmal, P.K. January 1, 2021-August 1, 2022. Determine the Efficacy of Closed Suction Drain After Hydrocelectomy. (END Trial) (END). ClinicalTrials.gov Identifier: NCT04653402 https://clinicaltrials.gov/ct2/show/NCT04653402

